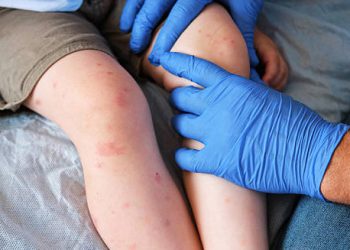
The diagnosis of hidradenitis suppurativa relies primarily on clinical evaluation rather than laboratory tests or imaging.
Early diagnosis helps people feel better sooner. It also lowers the risk of lasting skin damage. But many doctors miss the signs early on. This happens because hidradenitis suppurativa often looks like other common skin problems. These include boils, infected cysts, or acne. As a result, patients may go through many visits and failed treatments before learning what they truly have.
Many people feel frustrated before getting the correct diagnosis. They may feel alone or think the condition is their fault. That’s why raising awareness is so important. Both patients and healthcare providers need to know what to look for.
How Doctors Diagnose Hidradenitis Suppurativa
In most cases, the diagnosis of hidradenitis suppurativa starts with a physical exam and a medical history. There are no special blood tests or skin samples that can confirm it. Doctors rely on what they see and what the patient describes.
They pay close attention to the number, type, and location of bumps. They also ask how long the flare-ups last and how often they return. Painful lumps that keep coming back in areas like the underarms, groin, thighs, buttocks, or under the breasts raise a red flag—especially if these bumps keep appearing for over six months.
Doctors look for patterns. If the same spots flare up again and again, the condition may be chronic. The presence of tunneling under the skin or scarring supports the diagnosis. These features also help the doctor figure out how far the disease has progressed.
Symptoms and Family History Matter
The doctor will ask about other symptoms like pain, pus or blood leaks, or bad smells. They may also ask if anyone else in the family has similar symptoms. That’s because hidradenitis suppurativa often runs in families.
Doctors might ask about hormone levels, menstrual cycles, smoking, and weight. These all play a role. Conditions like polycystic ovary syndrome or Crohn’s disease often show up alongside hidradenitis suppurativa. So, doctors take a broad look at the patient’s overall health.
What the Doctor Looks For
During the exam, the doctor checks both current and past signs of the disease. These include thickened skin, dark marks, or scars. Where the lesions appear makes a big difference. If bumps are located in the underarms, groin, near the anus, or under the breasts, that points to hidradenitis suppurativa.
These bumps often return in the same places and form networks under the skin. That’s very different from a normal skin infection or pimple. Simple infections don’t form tunnels or come back in the same way.
Focus keyphrase: hidradenitis suppurativa
Understanding the Hurley Staging System
Doctors often use a tool called the Hurley staging system. It helps them sort the disease into mild, moderate, or severe:
- Stage I: One or more separate abscesses. No scarring or tunnels.
- Stage II: Repeat abscesses. Some scarring and tunnel-like tracts in more than one area.
- Stage III: Large areas involved. Many tunnels and lots of scar tissue.
This system helps guide treatment. It also helps the patient understand the severity of the disease.
Tests That Support the Diagnosis
Doctors usually don’t need scans or lab work to make a diagnosis. But in unclear cases, they may order tests. An ultrasound can help find tunnels or infected pockets deep in the skin. MRI scans also work but are used less often.
Blood tests don’t confirm hidradenitis suppurativa, but they can check for infection or rule out other issues. If the white blood cell count is high, that might show an infection during a flare-up. In more serious cases, doctors may check for inflammation using tests like CRP or ESR. These results are not specific to hidradenitis suppurativa but can help build the bigger picture.
Sometimes, a doctor may swab the skin if they think bacteria have caused a secondary infection. Still, these bacteria are not the main reason for the disease. They just make the problem worse.
Ruling Out Other Skin Conditions
Since the symptoms look like many other skin problems, doctors must rule out similar conditions. These include:
- Furunculosis: multiple infected hair follicles
- Pilonidal sinus: common at the base of the spine
- Cutaneous Crohn’s disease
- Infected cysts
- Acne inversa: a name sometimes used for hidradenitis suppurativa, but not always the same
If normal acne medicine or antibiotics don’t work, that’s another clue. Hidradenitis suppurativa often ignores standard treatments. When this happens, it sets the condition apart from others.
Creating a Supportive Space for Diagnosis
The process of diagnosing hidradenitis suppurativa must be kind and respectful. Many people feel shame or emotional pain. They may have lived with the symptoms for years. A supportive and non-judgmental doctor can make a big difference.
Open conversations lead to better care. When patients feel safe, they are more likely to stick to treatment plans. This trust is key for long-term care.
Focus keyphrase: hidradenitis suppurativa
Growing Awareness and Early Diagnosis
In recent years, people have learned more about hidradenitis suppurativa. More doctors now know how to spot it early. Education campaigns, social media, and training for dermatologists have helped a lot.
Still, many people stay silent. They may not talk about the symptoms because of embarrassment. Others may believe false ideas—like thinking the condition is caused by poor hygiene.
This is why public awareness matters so much. The more people know, the faster they can get help.
Final Thoughts on Diagnosis of Hidradenitis Suppurativa
To sum up, the diagnosis of hidradenitis suppurativa depends on spotting a clear pattern. This pattern includes painful, repeating bumps in key areas of the body. It also involves long-term skin changes like scarring or tunnels.
Lab tests and scans may help, but they are not always needed. The doctor’s trained eye and the patient’s story are often enough.
Early diagnosis leads to better results. It helps avoid lasting skin damage and brings faster relief. With care, education, and support, patients can move toward a better quality of life.