Hypoglycaemia is a clinical condition where blood glucose levels fall below normal, leading to a wide range of symptoms and potentially serious complications. Accurate diagnosis is essential not only for treating acute episodes but also for uncovering the underlying causes, especially in non-diabetic individuals.
Understanding Whipple’s Triad
Whipple’s Triad is the key framework doctors use to diagnose hypoglycaemia. It has three parts:
- Symptoms of low blood sugar
- Confirmed low blood glucose (usually below 3.0 mmol/L or 54 mg/dL)
- Relief of symptoms after eating or drinking glucose
This triad proves the symptoms come from hypoglycaemia and not other problems like anxiety or medication effects. It is especially helpful when symptoms come and go or are unclear.
Confirming Low Blood Glucose
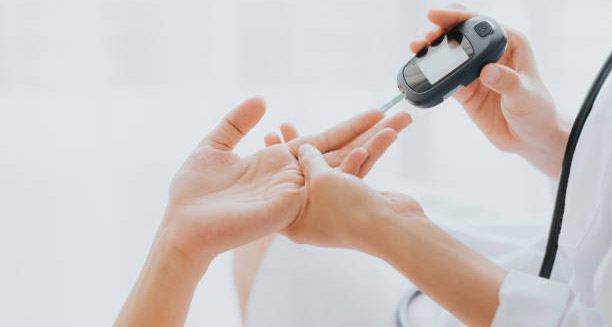
Doctors must measure blood sugar during symptoms. This happens through finger-prick tests or blood samples taken from a vein. Venous plasma glucose tests are more accurate and preferred. A reading under 3.0 mmol/L (54 mg/dL) generally shows clinically important hypoglycaemia, but this can vary for children or older adults.
If symptoms improve after glucose is given—through food, drink, or IV—it supports the diagnosis of hypoglycaemia.
Taking a Medical History
A detailed medical history helps find possible causes. Important details include:
- Type of diabetes and medicines used
- Meal timing, missed meals, or fasting
- Exercise habits and unusual physical activity
- Alcohol use and timing related to symptoms
- Other medications like beta-blockers or quinine
- Family history of genetic or metabolic problems
Knowing when symptoms happen is also useful. For example, episodes a few hours after eating may suggest reactive hypoglycaemia. Episodes during sleep might relate to nocturnal hypoglycaemia or alcohol use.
Investigating Underlying Causes
After confirming hypoglycaemia, doctors look for its cause. This can be complex, especially without diabetes.
Supervised Fasting Test
If episodes are rare or hard to catch, a 72-hour fast under medical supervision may be used. Blood tests for glucose, insulin, and other markers happen regularly or when symptoms appear. This test helps find insulinomas (insulin-producing tumors), fake hypoglycaemia caused by hidden insulin or drug use, and hormone problems like adrenal insufficiency.
High insulin with low C-peptide suggests injected insulin. High insulin with high C-peptide points to excess natural insulin, as seen in insulinomas or sulfonylurea use.
Mixed-Meal Tolerance Test (MMTT)
To diagnose reactive hypoglycaemia, the patient eats a carb-rich meal. Blood sugar is then checked over several hours. A delayed drop confirms the diagnosis.
Hormonal and Metabolic Tests
If hormone problems are suspected, doctors check:
- Cortisol for adrenal problems
- Growth hormone, especially in children with repeated episodes
- Liver and kidney function to assess glucose production and medicine clearance
- Serum ketones and free fatty acids for metabolic disorders
- Lactate levels for rare metabolic diseases
These tests are usually ordered by endocrinologists when hypoglycaemia is unexplained or comes back often.
Continuous Glucose Monitoring (CGM)
CGMs are wearable devices that track glucose levels continuously. They help:
- People with diabetes prone to frequent or severe lows
- Those who don’t feel early symptoms (hypoglycaemia unawareness)
- Children who cannot clearly describe symptoms
- Night-time monitoring to catch nocturnal hypoglycaemia
CGMs give detailed graphs and alerts, spotting trends missed by finger-prick checks. Some link to insulin pumps to adjust insulin automatically and prevent dangerous lows.
Considering Other Causes
Not all symptoms like hypoglycaemia come from low blood sugar. Doctors consider:
- Anxiety or panic attacks
- Irregular heart rhythms
- Seizures
- Mini strokes (transient ischemic attacks)
- Migraine auras
Matching symptoms to blood glucose levels and checking if glucose fixes symptoms helps rule out these other causes.
Diagnosing Hypoglycaemia in Children
Children, especially newborns, have different glucose limits and causes. Diagnosis includes:
- Using age-specific glucose cutoffs (below 2.6 mmol/L in newborns is worrying)
- Testing for inherited metabolism problems like glycogen storage disease
- Screening for hormone deficiencies such as cortisol or growth hormone
Blood tests need to be done quickly because children’s glucose can change fast. Doctors, pediatricians, and metabolic specialists work closely in these cases.
Functional vs. Pathological Hypoglycaemia
Doctors separate functional hypoglycaemia (like reactive or fasting-related) from pathological causes. Functional types often improve with diet changes. Pathological causes need deeper tests and sometimes lifelong treatment. This difference is based on symptom timing, other health issues, and test results.
Conclusion
The diagnosis of hypoglycaemia requires more than just finding low blood sugar. Doctors use Whipple’s Triad, review risk factors, examine episode context, and apply lab and monitoring tools to find the cause. Diagnosis is simpler in people with diabetes but more detailed in others. A correct diagnosis leads to better care, fewer future episodes, and improved quality of life.
Diagnosis of hypoglycaemia sets the path for safe and effective treatment.