Diagnosis of Corticobasal Degeneration
Diagnosis of corticobasal degeneration is often difficult, especially in the early stages, due to the overlap of symptoms with other neurological disorders. There is no single test that can definitively confirm corticobasal degeneration during life. Instead, diagnosis is made through a combination of clinical assessments, neurological examinations, and imaging studies that help rule out other possible conditions.
Medical History and Clinical Assessment
The process typically begins with a thorough evaluation of:
Onset and progression of symptoms
Degree of asymmetry in movement difficulties
Cognitive and behavioural changes
Speech and swallowing problems
Doctors will look for the combination of movement and cognitive symptoms that are characteristic of corticobasal degeneration, especially unilateral stiffness, apraxia, and speech changes.
Neurological Examination | Diagnosis of Corticobasal Degeneration
A neurologist will assess:
Muscle tone and reflexes
Coordination and balance
Ability to perform learned movements
Memory, attention, and language function
Findings such as limb rigidity, difficulty performing simple tasks despite adequate strength, and alien limb syndrome are suggestive of corticobasal degeneration.
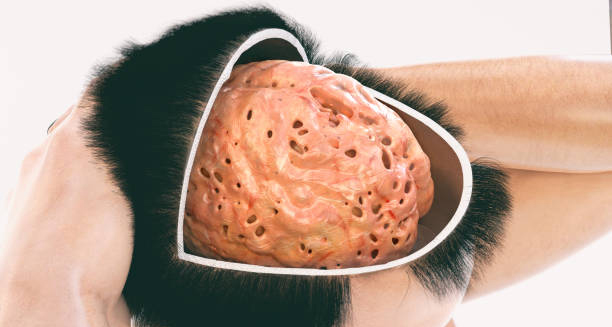
Brain Imaging
MRI scans may show shrinkage (atrophy) in specific brain areas such as the parietal lobe or frontal cortex, often more pronounced on one side.
PET or SPECT scans can assess metabolic activity and highlight regions of the brain that are underactive due to nerve cell damage.
These imaging results support the diagnosis and help differentiate corticobasal degeneration from Parkinson’s disease, Alzheimer’s, or progressive supranuclear palsy.
Neuropsychological Testing
This type of testing evaluates memory, attention, problem-solving, and language skills. It helps identify cognitive decline patterns typical of corticobasal degeneration.
Exclusion of Other Conditions | Diagnosis of Corticobasal Degeneration
Because symptoms overlap with other disorders, conditions such as Parkinson’s disease, frontotemporal dementia, or stroke must be ruled out. Blood tests and, in rare cases, lumbar puncture may be conducted to exclude other causes.
In summary, diagnosis of corticobasal degeneration relies on clinical expertise, symptom observation, and supportive imaging. Due to the lack of a specific test, ongoing reassessment is often necessary to confirm the condition over time.
[Next: Treatment of Corticobasal Degeneration →]