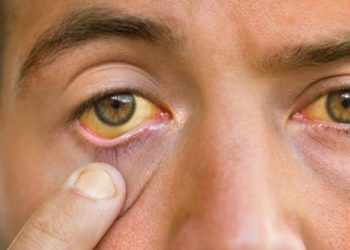
Diagnosing isovaleric acidaemia can be challenging, particularly due to its rarity and the non-specific nature of many early symptoms. The condition often looks like common illnesses such as sepsis, stomach infections, or brain disorders in newborns and young children. However, as awareness grows and newborn screening expands, detecting isovaleric acidaemia early has become easier.
This section explains how doctors diagnose this condition through clinical signs, lab tests, genetic checks, and newborn screening. Early diagnosis helps prevent metabolic crises and allows timely treatment, which improves long-term health.
Clinical Suspicion and History Taking
Doctors first suspect isovaleric acidaemia when infants show symptoms like poor feeding, tiredness, vomiting, seizures, or unexplained acid buildup in the blood. A “sweaty feet” smell is also a key clue. Family history matters too. If siblings have the condition or parents are related, the chance of inherited metabolic disease rises. Symptoms that start after eating protein may also hint at this disorder.
Because these signs overlap with infections or birth injuries, doctors may not think of isovaleric acidaemia at first. But when blood tests show metabolic acidosis with a high anion gap, ketosis, and low blood sugar, metabolic disorders must be considered.
Biochemical Testing
After suspicion, lab tests confirm the diagnosis by measuring toxic substances from broken-down leucine.
a. Plasma Acylcarnitine Profile
This blood test checks for high levels of isovalerylcarnitine (C5), which is a clear sign of isovaleric acidaemia. It is often done on dried blood spots during newborn screening.
b. Urine Organic Acid Analysis
Testing urine shows raised amounts of isovalerylglycine, isovaleric acid, and related compounds, which strongly indicate the condition.
c. Blood Ammonia and Lactate
High ammonia and lactate levels may appear during crises. These markers help doctors understand the crisis severity and plan treatment.
d. Arterial Blood Gases and Anion Gap
Metabolic acidosis with a raised anion gap means organic acids build up in blood, prompting more metabolic tests.
e. Serum Glucose and Ketones
Low blood sugar and ketones may also appear during stress, supporting the diagnosis.
Genetic Testing
Definitive diagnosis comes from finding mutations in the IVD gene on chromosome 15. This gene controls the enzyme that breaks down isovaleryl-CoA.
- If a family mutation is known, targeted testing finds it quickly.
- Full gene sequencing finds new or mixed mutations.
Genetic tests confirm the diagnosis and allow screening of family members and prenatal testing. Some populations have common mutations, which makes testing easier.
Newborn Screening
Many countries test newborns for isovaleric acidaemia using tandem mass spectrometry on dried blood spots. This test detects high C5 acylcarnitines within days after birth.
Early screening helps by:
- Preventing dangerous metabolic crises in newborns
- Starting diet and supplements early
- Offering genetic counselling
- Improving long-term brain development
However, screening can give false positives or negatives, especially in mild cases or premature babies. Abnormal results need further biochemical and genetic checks.
Differential Diagnosis
Symptoms and lab results in isovaleric acidaemia can resemble other metabolic diseases like:
- Propionic acidaemia
- Methylmalonic acidaemia
- Maple syrup urine disease (MSUD)
- Multiple acyl-CoA dehydrogenase deficiency (MADD)
- Sepsis or neonatal brain injury
Doctors use biochemical markers and genetic tests to tell these apart. For example, isovalerylglycine in urine points to isovaleric acidaemia, while other acids suggest different disorders.
Prenatal Diagnosis
Families with a history of isovaleric acidaemia may choose prenatal testing by chorionic villus sampling or amniocentesis. These tests check the fetus for defective IVD genes using:
- Genetic analysis of fetal DNA
- Sometimes enzyme activity tests in fetal tissue
These help families prepare for medical care and early treatment after birth.
Enzyme Assays
Although rare now, doctors can measure isovaleryl-CoA dehydrogenase activity in cells from skin or blood. Low or absent activity confirms the diagnosis. This method is mostly used in research or where genetic testing is unavailable.
Family Testing and Cascade Screening
After diagnosis, doctors recommend testing siblings and relatives. Finding carriers or affected people early helps start care and lower risks. Sometimes siblings have mild or no symptoms but still carry the condition.
Conclusion
Diagnosing isovaleric acidaemia takes clinical awareness, lab tests, genetic analysis, and newborn screening. Though early symptoms may mimic common newborn illnesses, signs like the sweaty feet smell, metabolic acidosis, and high C5 acylcarnitines guide doctors to the right diagnosis.
Timely diagnosis saves lives by enabling quick treatment and preventing brain damage. As newborn screening spreads, early detection and care improve, giving hope to families facing this rare but serious disorder.