Diagnosis of Mastocytosis
Diagnosis of Mastocytosis can be a complex and meticulous process due to the rarity of the condition and its diverse clinical presentation.
Clinicians start by suspecting it when seeing skin lesions, unexplained allergic reactions, or systemic signs like stomach pain, tiredness, or anaphylaxis. Because mastocytosis appears differently in children versus adults—and can be either cutaneous or systemic—doctors must take a detailed medical history and follow a step‑by‑step diagnostic plan to find and label the disease correctly.
Mastocytosis involves too many mast cells building up in different tissues. In children, it often stays on the skin (cutaneous forms). In adults, it tends to affect organs like bone marrow, liver, spleen, or the gut (systemic forms). Thus, the diagnostic path changes depending on which type doctors suspect. A child with only skin spots might only need skin tests, while an adult with systemic signs may need complex blood and bone marrow tests.
Clinical Evaluation and Medical History
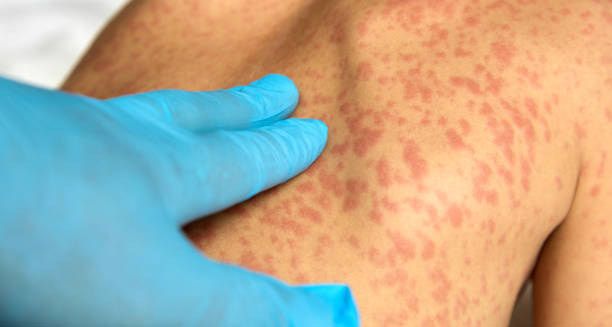
Doctors begin by carefully examining the patient’s skin. They look for reddish‑brown patches or spots that swell or itch when rubbed. This reaction is called Darier’s sign, and it often signals cutaneous mastocytosis.
Then they interview the patient about symptoms. They ask how often allergic reactions occur, whether there is diarrhoea or abdominal pain, episodes of low blood pressure, headaches, bone pain, or unexplained tiredness. A family history of similar symptoms or rare genetic illnesses can guide the diagnosis. This history helps them tell mastocytosis apart from other allergies or blood diseases with similar signs.
If symptoms affect internal systems—like chronic gut issues, flushing, or repeated anaphylaxis with no clear cause—doctors will proceed with lab tests and possibly imaging scans.
Blood Tests and Serum Tryptase Levels
A key lab test is the serum tryptase level. Tryptase is an enzyme that mast cells release, and elevated levels often reflect excess mast cells. A baseline tryptase above ~20 ng/mL strongly suggests mast cell overgrowth and signals need for further testing.
But a high tryptase is not unique to mastocytosis. It also occurs in allergic reactions, kidney disease, or certain blood disorders. That means tryptase alone can’t confirm the disease—it just adds a piece to the puzzle.
Routine blood counts may show signs of bone marrow involvement, such as increased eosinophils, low red cells (anaemia), or low platelets (thrombocytopenia). If those appear, doctors may send the patient to a haematologist for deeper investigations.
Skin Biopsy for Cutaneous Mastocytosis
When cutaneous mastocytosis is suspected, doctors may take a skin sample (biopsy) under local anaesthetic. A pathologist examines this under a microscope using stains that highlight mast cells.
They look for clusters of mast cells in the dermis, often near blood vessels. They also use immunohistochemical stains for markers like CD117 (c-KIT) and tryptase to confirm the presence of mast cells. This method often suffices to diagnose cutaneous mastocytosis, especially in children, without further invasive tests.
Bone Marrow Biopsy and Histology
If doctors suspect systemic mastocytosis—especially in adults or people with high tryptase and multi-organ signs—they will recommend a bone marrow biopsy.
This sample usually comes from the pelvic bone, often under local anaesthetic. Specialists examine it for mast cell count, clustering, and shape. In systemic mastocytosis, many mast cells become spindle‑shaped. If they find clusters of 15 or more mast cells in marrow, that meets one of the major WHO criteria.
The biopsy also checks for other blood abnormalities, because systemic mastocytosis often co-occurs with diseases like chronic myelogenous leukaemia or myelodysplastic syndromes.
Genetic Testing: KIT Mutations
Testing for gene changes is a crucial part of the diagnostic process. A common mutation in mastocytosis is KIT D816V, which causes uncontrolled mast cell growth.
Doctors test for this mutation using material from bone marrow, blood, or sometimes skin. A positive result offers strong molecular proof of systemic mastocytosis. It also helps guide treatment, since some targeted drugs don’t work well in cases with that mutation.
Testing for KIT mutations doesn’t just confirm diagnosis. It helps separate systemic mastocytosis from other clonal disorders. The presence of additional mutations (such as in SRSF2 or ASXL1) may point to a more aggressive disease course.
Diagnostic Criteria by the WHO
The WHO defines specific rules to confirm systemic mastocytosis. The patient must meet:
- One major criterion
- One minor criterion
OR - At least three minor criteria
Major Criterion:
- Dense clusters (≥ 15 mast cells) in bone marrow or other organs outside skin
Minor Criteria:
- Over 25% of mast cells in those clusters have spindle‑shaped or atypical forms
- Detection of the KIT D816V mutation
- Expression of CD2 and/or CD25 in addition to normal mast cell markers (e.g. CD117)
- Persistent serum tryptase above 20 ng/mL (if no other cause)
These criteria aim to ensure that doctors worldwide follow a standard method. They also reduce misdiagnosis, especially between mastocytosis and similar conditions like mast cell activation syndrome (MCAS).
Imaging Studies
Although not required in every case, imaging tests help assess organ involvement. Doctors may order abdominal ultrasound, CT scans, or MRI if they suspect liver or spleen enlargement, lymph nodes, or bone lesions.
They may also do bone density scans (DEXA), since systemic mastocytosis can lead to thinning bones (osteopenia) or osteoporosis—especially in men and postmenopausal women.
Differential Diagnosis
Many conditions mimic mastocytosis, so doctors must rule them out. Some of these include:
- Chronic urticaria or other allergic disorders
- Mast cell activation syndrome (MCAS)
- Myeloproliferative diseases
- Lymphoma or leukaemia
- Eosinophilic gastrointestinal disorders
Thus, diagnosing mastocytosis involves not just identifying it, but also excluding other similar illnesses. A team of specialists—dermatologists, allergists, haematologists, and geneticists—often works together.
Final Thoughts on the Diagnostic Journey
The diagnosis of Mastocytosis is a detailed and layered process combining clinical judgment, lab tests, histology, and genetics. The disease can range from isolated skin involvement to aggressive systemic forms that damage many organs.
Detecting it early and accurately matters. It not only helps manage symptoms but also lowers the risk of dangerous outcomes like anaphylaxis, organ failure, or secondary blood cancers. Thanks to advances in genetic tests and unified diagnostic guidelines, clinicians are better able to find, classify, and treat this rare but serious condition.